Key to the Brain
Section titled “Key to the Brain”In this series of articles on brain aging, we have tried to unlock the mysteries the brain to help you understand how it works and what can go wrong. We've described how the delicate structure of nerves makes them prone to oxidation, a kind of rusting as we age. We've explored the mitochondria – the amazing bodies that power the brain and, at the same time, can cause destruction. We've traveled along the synaptic connections with the neurotransmittors and cringed watching the formation of brain-destroying plaque. This month, we will focus on a larger structure, the hippocampus, seat of memory and spatial orientation. It's important to understand the function of the hippocampus, but even more important, the study of this region of the brain takes us to an exciting subject – the brain's ability to regenerate and renew itself.
The Seahorse in the Brain
Section titled “The Seahorse in the Brain”There is a seahorse in the brain, called the hippocampus, from the Greek for “seahorse”. The illustration below shows the seahorse shape, while the red rectangle in the CT image shows the location of the hippocampus. (In the large image, the brain is shown in grey, superimposed over a whitish background with a shadow. The "seahorse" faces left.)
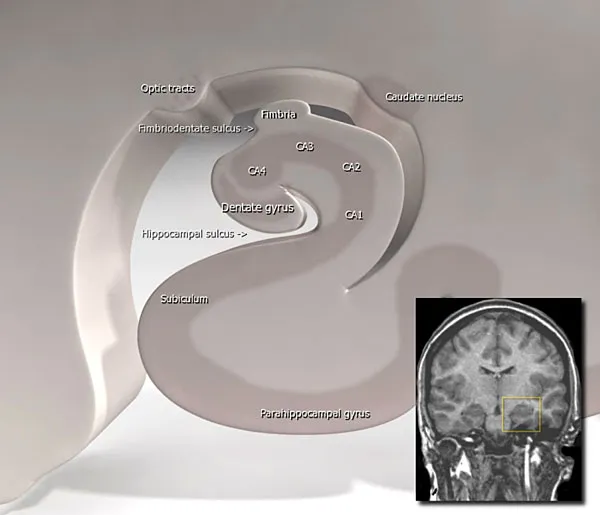
Figure 1: The Hippocampus
The beautiful hippocampus promotes memory and spatial orientation. Since Alzheimer's especially affects the hippocampus, memory and navigation are the first faculties people with Alzheimer's lose.
The hippocampus is uniquely susceptible to damage from stress. Researchers at McGill University in Quebec followed people for five years. Those who coped poorly with stress had shrinkage of the hippocampus and loss of memory and other functions.1 Let's see what happens in the brain when we deal with stress.
Neuroplasticity: The Secret's in the Stem Cell
Section titled “Neuroplasticity: The Secret's in the Stem Cell”Time was, we were taught that brain cells were irreplaceable. While we could grow new skin cells or lining cells for the gastrointestinal tract, brain cells were all created before birth. Then we learned that stroke victims regained function best when they were returned to activity quickly after the stroke -- and that gave us the first clue that the brain might be able to reg enerate. Before, we let the stroke victim rest and get out of bed when and if they felt they were able. Many times, they were never able to walk again. Now stroke victims go to special rehabilitation centers where they are more-or-less forced to walk long before they think they can. We've learned that recovery from stroke is much more complete this way.
A stroke results from damaged brain tissue. Most often a clot blocks a major brain artery, and within minutes the brain tissue sustained by that artery begins to die. (Sometimes the damage results from bleeding; the symptoms are often similar, the medication quite different; the benefit from rapid return to activity the same.) Once that particular chunk of brain dies, that's it. It's not coming back. But the brain tissue just next to it can take over its function. We call this neuroplasticity, meaning that the adjacent tissue remodels itself to take over the function of the destroyed tissue. How is this possible?
Researchers have found that the brain contains stem cells. Stems cells have the ability to divide and form themselves into other, specialized cells. For example, at conception, the ovum can be considered a stem cell; it will divide and the daughters will differentiate themselves into kidney cells, skin cells, blood cells, brain cells, and all the other tissues of the body. The bone marrow of an adult contains stem cells, which have no other purpose than to divide and provide daughter cells that become red blood cells and all the different kinds of white blood cells. A careful search of the brain has, in recent years, uncovered stem cells that can, when encouraged, divide and change into neurons and glial cells.
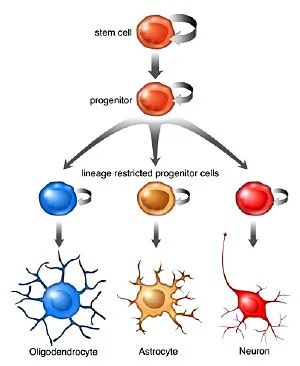
In this image, a stem cell is shown capable of generating different kinds of brain cells depending upon need, either a neuron, or a glial cell such as an oligodendrocyte or an astrocyte. The production of new brain cells is called neurogenesis. The process by which these cells interact with existing brain cells to recreate the function of damaged brain tissue is called neuroplasticity. 2
Neurotrophins Enable the Birth of New Cells
Section titled “Neurotrophins Enable the Birth of New Cells”While we have but recently discovered that the brain can grow new cells, we've known for some time that the synapses that connect cells form new connections and lose old ones all our lives. This is part of the process of learning, be it physical, mental, or emotional, and it occurs through the mediation of brain-tissue growth factors called neurotrophins (“trophin” from a Greek word meaning birth). These neurotrophins are produced as a result of brain activity and have a more important role in certain areas of the brain, including the frontal cortex and hippocampus.
One of the better known among the many different neurotrophins is brain derived neurotrophic factor (BDNF). It contributes not just to the synaptic reconnections, but also to neurogenesis, the growth of new cells. . BDNF helps us form our brain after birth and as we grow3. BDNF is critically important to the hippocampus. Perhaps it shouldn't be a surprise that levels of BDNF are low in people wit h Alzheimer's
Brain Regeneration
Section titled “Brain Regeneration”This process of brain regeneration is a product of stem cells and of nerve growth factors. These two processes require physical activity and mental activity to work. This is why stroke victims regain function better when forced into medical boot camp. Animal studies show that the hippocampus regenerates itself twice as well when given learning tasks.4 Take away stimulation, and the brain does not regenerate. This is why animals grown in the dark lose vision, because the neurotrophins that sustain optic nerves aren't produced without stimulation. Similarly, people with less mental stimulation are more likely to develop Alzheimer's. Less learning-stimulated nerve activity in the frontal cortex and hippocampus means less neurotrophic activity in the hippocampus. As activity decreases, researchers see shrinkage of the cortex and the beautiful seahorse in the brains of people with Alzheimer's.
By the way, neurotrophins do not cross the blood-brain barrier, so don't look for a pill. The only way to stimulate neurotrophins is to exercise your noggin.
Depression and the Brain
Section titled “Depression and the Brain”The hippocampus is part of the limbic system involved with emotion. Depression and other mood disorders have been linked to decreased neurogenesis in the hippocampus. There is evidence that increasing hippocampal neurogenesis through exercise reduces depression.5 Research also shows that the mental stimulation provided by other humans is more effective than mental stimulation in isolation.6 Studies also show that exposing laboratory animals to various external stressors enhances the production of BDNF among other nerve protective factors, so that when the animal is subsequently stressed, the nerve tissue is less likely to be harmed as a result of that stress. Conversely, if the animal is never challenged, when it finally is faced with some stressor, the brain tissue will be more likely to succumb to apoptosis and other neurodegenerative processes..7 We are not born to be raised in hothouses, nor to live in them. Exposing ourselves to the challenges of vigorous living makes our brains more robust.
Alcohol and the Brain
Section titled “Alcohol and the Brain”In low doses, one or two ounces a day, alcohol appears to benefit short-term memory and problem solving ability. We're talking about long-term benefits; don't make a major decision after a couple of beers. In higher doses, however, alcohol poisons the brain. Long has it been known that heavy drinkers lose mental function over the long term. Now we know why. Alcohol interferes with neurogenesis.
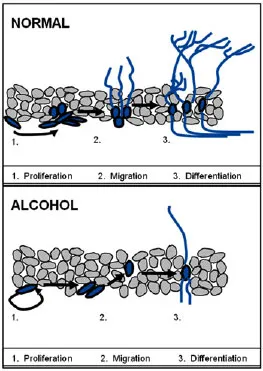
Figure 3: Neurogenesis in the normal and alcohol-soaked brain
The upper image shows a normal brain. Neuroregenerative processes in the brain respond to demand, which comes from exercise or the effort to learn. With the help of neurotrophic factors, the stem cells on the left increase in number and migrate to the area of need. Then they transform themselves into neurons or glial cells as required. The brain thus continues to mature and develop as we expect it to do.
But look what happens with excessive alcohol. Stem cells do not increase as much in number and do not form as many neurons (the blue lines above the label "3. differentiation "). Just when individuals most need critical thinking to help them change their lives, they have the least ability. This is why treatment programs must last from one to several months, to allow brain function to return to normal. Only then will the individual have a chance at sobriety.
Summary: Your Wonderful Brain
Section titled “Summary: Your Wonderful Brain”Your brain is subject to damage through the normal slings and arrows of time. In most cases, it has the ability to repair itself if you take good care of it. This month we've looked specifically at the brain's ability to form new cells that will replace those that have been damaged. This is good news and a good reason not to give up and accept dimming memory and abilities as a part of life. When you exercise your mind and your body, you give your brain what it needs to form new cells and new synapses. Sure, and you're not likely to be the exception to the general rule that we all return to dust, but you can make the best of what you are given. My wish for you is that you can be that sharp, snappy, respected elder, still loved and valued by your friends and family.
Coming Soon
Section titled “Coming Soon”As we've reviewed brain function in this series of newsletters, I have mentioned various factors that improve brain function. In the next newsletter, I will survey supplements you may have seen touted as “anti-aging,” together with the research that supports or refutes their claims.
In the final newsletter of this series, I will corral all this information into a series of practical recommendations for maintaining healthy brain function as you age.
Endnotes:
1 Cortisol levels during human aging predict hippocampal atrophy and memory deficits. Nat Neurosci 1998 May;1(1):69-73
Douglas Hospital Research Center, Department of Psychiatry, McGill University, Verdun, Québec, Canada.
Elevated glucocorticoid levels produce hippocampal dysfunction and correlate with individual deficits in spatial learning in aged rats. Previously we related persistent cortisol increases to memory impairments in elderly humans studied over five years. Here we demonstrate that aged humans with significant prolonged cortisol elevations showed reduced hippocampal volume and deficits in hippocampus-dependent memory tasks compared to normal-cortisol controls. Moreover, the degree of hippocampal atrophy correla ted strongly with both the degree of cortisol elevation over time and current basal cortisol levels. Therefore, basal cortisol elevation may cause hippocampal damage and impair hippocampus-dependent learning and memory in humans.
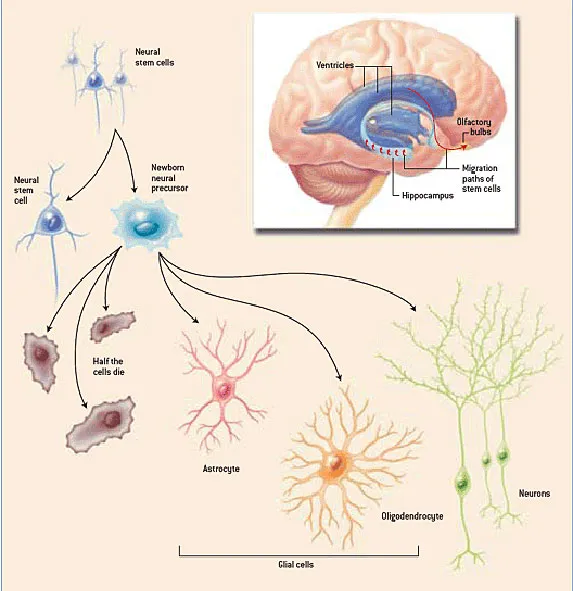
Source: http://pages.slc.edu/~ebj/iminds04/L7-neuroplasticity/gage.htm
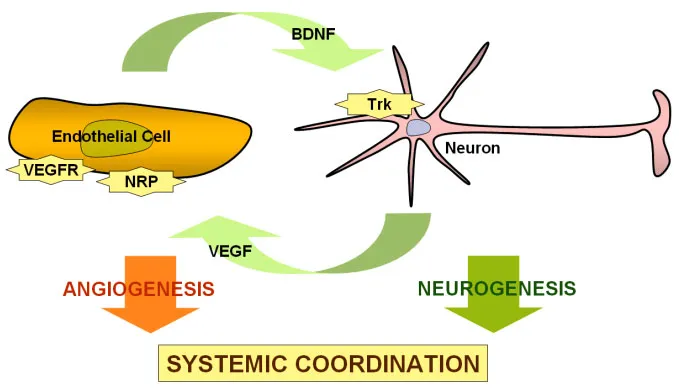
Source: http://angiodb.snu.ac.kr/arl/re_field/milibiology.php
This schematic diagram shows how the lining cells of the blood vessels of the brain, the endothelial cells, secrete BDNF to stimulate neurogenesis, growth and development of neurons. Neurons in turn secrete vascular-endothelial growth factor to promote angiogenesis, the growth of new blood vessels to bring blood to newly developed nerve tissue. Trk and NRP are other substances involved in the process, and beyond the scope of this discussion.
4 Learning enhances adult neurogenesis in the hippocampal formation. Nat Neurosci 1999 Mar;2(3):260-5
Department of Psychology, Princeton University, Princeton, New Jersey 08544, USA.
Thousands of hippocampal neurons are born in adulthood, suggesting that new cells could be important for hippocampal function. To determine whether hippocampus-dependent learning affects adult-generated neurons, we examined the fate of new cells labeled with the thymidine analog bromodeoxyuridine following specific behavioral tasks. Here we report that the number of adult-generated neurons doubles in the rat dentate gyrus in response to training on associative learning tasks that require the hippocampus. In contrast, training on associative learning tasks that do not require the hippocampus did not alter the number of new cells. These findings indicate that adult-generated hippocampal neurons are specifically affected by, and potentially involved in, associative memory formation.
5 Antidepressant effects of exercise: evidence for an adult-neurogenesis hypothesis? J Psychiatry Neurosci 2006 Mar;31(2):84-92
Neuroscience Program, UBC Hospital, University of British Columbia, Vancouver, BC.
It has been hypothesized that a decrease in the synthesis of new neurons in the adult hippocampus might be linked to major depressive disorder (MDD). This hypothesis arose after it was discovered that antidepressant medications increased the synthesis of new neurons in the brain, and it was noted that the therapeutic effects of antidepressants occurred over a time span that approximates the time taken for the new neurons to become functional. Like antidepressants, exercise also increases the synthesis of new neurons in the adult brain: a 2-3-fold increase in hippocampal neurogenesis has been observed in rats with regular access to a running wheel when they are compared with control animals. We hypothesized, based on the adult-neurogenesis hypothesis of MDD, that exercise should alleviate the symptoms of MDD and that potential mechanisms should exist to explain this therapeutic effect. Accordingly, we evaluated studies that suggest that exercise is an effective treatment for MDD, and we explored potential mechanisms that could link adult neurogenesis, exercise and MDD. We conclude that there is evidence to support the hypothesis that exercise alleviates MDD and that several mechanisms exist that could mediate this effect through adult neurogenesis.
6 Environmental complexity and central nervous system development and function. Ment Retard Dev Disabil Res Rev 2004;10(2):91-5
McKnight Brain Institute and Department of Psychiatry, University of Florida, Gainesville, Florida 32601, USA. mlewis@psychiatry.ufl.edu
Environmental restriction or deprivation early in development can induce social, cognitive, affective, and motor abnormalities similar to those associated with autism. Conversely, rearing animals in larger, more complex environments results in enhanced brain structure and function, including increased brain weight, dendritic branching, neurogenesis, gene expression, and improved learning and memory. Moreover, in animal models of CNS insult (e.g., gene deletion), a more complex environment has attenuated or prevented the sequelae of the insult. Of relevance is the prevention of seizures and attenuation of their neuropathological sequelae as a consequence of exposure to a more complex environment. Relatively little attention, however, has been given to the issue of sensitive periods associated with such effects, the relative importance of social versus inanimate stimulation, or the unique contribution of exercise. Our studies have examined the effects of environmental complexity on the development of the restricted, repetitive behavior commonly observed in individuals with autism. In this model, a more complex environment substantially attenuates the development of the spontaneous and persistent stereotypies observed in deer mice reared in standard laboratory cages. Our findings support a sensitive period for such effects and suggest that early enrichment may have persistent neuroprotective effects after the animal is returned to a standard cage environment. Attenuation or prevention of repetitive behavior by environmental complexity was associated with increased neuronal metabolic activity, increased dendritic spine density, and elevated neurotrophin (BDNF) levels in brain regions that are part of cortical-basal ganglia circuitry. These effects were not observed in limbic areas such as the hippocampus.
7 Prophylactic activation of neuroprotective stress response pathways by dietary and behavioral manipulations. NeuroRx 2004 Jan;1(1):111-6
Laboratory of Neurosciences, National Institute on Aging Gerontology Research Center, Baltimore, Maryland 21224, USA. mattsonm@grc.nia.nih.gov
It is well established that when most types of cells, including neurons, are exposed to a mild stress they increase their ability to resist more severe stress. This "preconditioning" phenomenon involves up-regulation of genes that encode cytoprotective proteins such as heat-shock proteins and growth factors. We found that a similar beneficial cellular stress response can be induced in neurons throughout the brain by a "meal-skipping" dietary restriction (DR) regimen in rats and mice. DR is effective in protecting neurons and improving functional outcome in models of stroke, Alzheimer's, Parkinson's and Huntington's diseases. DR induces an increase in the levels of brain-derived neurotrophic factor (BDNF) and heat-shock proteins in neurons. DR also stimulates neurogenesis in the hippocampus, and BDNF plays a role in this effect of DR. Physical exercise and environmental enrichment are two other manipulations that have been shown to induce BDNF expression in the brain, presumably because it is a mild cellular stress. When taken together with epidemiological and clinical studies in humans, the data from animal studies suggest that it may be possible to reduce the risk for age-related neurodegenerative disorders through dietary and behavioral modifications that act by promoting neuronal plasticity and survival.